
Members were paying for insurance they didn't fully understand — and couldn't easily manage. That's not just a UX problem. It's a trust problem.
AMA's insurance products — auto, home, life, travel — were managed across a patchwork of disconnected portals, each with its own login, terminology, and visual language. Members couldn't see all their policies in one place, couldn't easily make changes, and often didn't know what they were actually covered for without calling an agent. This friction drove up contact centre volume and eroded confidence in the brand.
My mandate: Design a unified insurance portal that gave members clarity, control, and confidence over their coverage — all in one authenticated experience.
"Insurance is inherently complex — but complexity is never an excuse for poor design. Our job was to absorb the complexity so members didn't have to."
Ran workshops with insurance product owners, legal, and front-line agents to map the full policy management landscape and regulatory constraints.
Interviewed members across coverage types — from first-time auto buyers to long-term home insurance holders — uncovering mental models and pain points.
Worked with content strategists to rewrite insurance terminology into plain language — every label, heading, and help text reviewed for clarity.
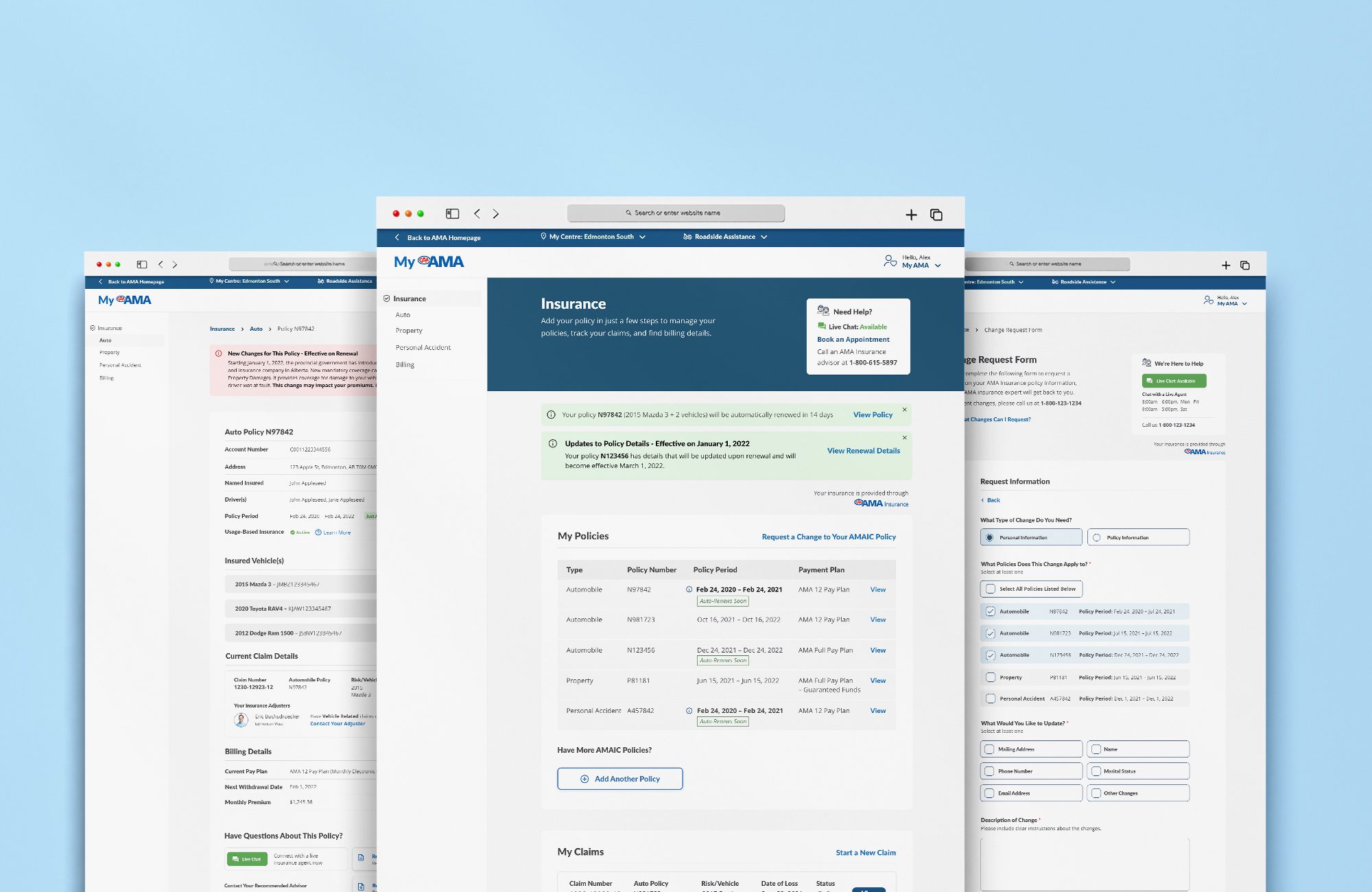
Designed a unified dashboard, policy detail views, claims tracking, and document centre — all tested with members across 3 prototype rounds.
The MyAMA Insurance portal launched as a single authenticated destination for all AMA insurance products. Members could see every active policy, coverage details, and upcoming renewals in one dashboard view. Policy documents were downloadable, claims were trackable in real time, and common changes — updating a vehicle, adding a driver — could be initiated self-serve without calling an agent.
Key design decisions: A policy card system made coverage scannable at a glance. Plain-language coverage summaries replaced legal jargon. Smart alerts surfaced upcoming renewals and potential coverage gaps. The claims tracker brought transparency to a process that had previously felt like a black box.

Loading video…